ANGINA PECTORIS
 Angina pectoris, the primary symptom of ischemic heart disease, is caused by transient episodes of myocardial ischemia that are due to an imbalance in the myocardial oxygen supply-demand relationship. This imbalance may be caused by an increase in myocardial oxygen demand (which is determined by heart rate, ventricular contractility, and ventricular wall tension) or by a decrease in myocardial oxygen supply (primarily determined by coronary blood flow but occasionally modified by the oxygen-carrying capacity of the blood) or sometimes by both. Since blood flow is inversely proportional to the fourth power of the artery’s luminal radius, the progressive decrease in vessel radius that characterizes coronary atherosclerosis can impair coronary blood flow and lead to symptoms of angina when myocardial oxygen demand increases, as with exertion (so-called typical angina pectoris).
Angina pectoris, the primary symptom of ischemic heart disease, is caused by transient episodes of myocardial ischemia that are due to an imbalance in the myocardial oxygen supply-demand relationship. This imbalance may be caused by an increase in myocardial oxygen demand (which is determined by heart rate, ventricular contractility, and ventricular wall tension) or by a decrease in myocardial oxygen supply (primarily determined by coronary blood flow but occasionally modified by the oxygen-carrying capacity of the blood) or sometimes by both. Since blood flow is inversely proportional to the fourth power of the artery’s luminal radius, the progressive decrease in vessel radius that characterizes coronary atherosclerosis can impair coronary blood flow and lead to symptoms of angina when myocardial oxygen demand increases, as with exertion (so-called typical angina pectoris).
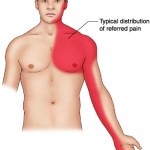
In some patients, anginal symptoms may occur without any increase in myocardial oxygen demand but rather as a consequence of abrupt reduction in blood flow, as might result from coronary thrombosis (unstable angina) or vasospasm (variant or Prinzmetal angina). Regardless of the precipitating factors, the sensation of angina is similar in most patients. Typical angina is experienced as a heavy, pressing sub sternal discomfort (rarely called “pain”), often radiating to the left shoulder, flexor aspect of the left arm, jaw, or epigastrium. However, a significant minority of patients notes discomfort in a different location or of a different character. Women, the elderly, and diabetics are more likely to have ischemia with atypical symptoms. In most patients with typical angina, whose symptoms are provoked by exertion, the symptoms are relieved by rest or by administration of sublingual nitro-glycerine.
Angina pectoris is a common symptom, affecting more than 6 million Americans. Angina pectoris may occur in a stable pattern over many years or may become unstable, increasing in frequency or severity and even occurring at rest. In typical stable angina, the pathological substrate is usually fixed atherosclerotic narrowing of an epicardial coronary artery, on which exertion or emotional stress superimposes an increase in myocardial oxygen consumption. In variant angina, focal or diffuse coronary vasospasm episodically reduces coronary flow. Patients also may display a mixed pattern of angina with the addition of altered vessel tone on a background of atherosclerotic narrowing. In most patients with unstable angina, rupture of an atherosclerotic plaque, with consequent platelet adhesion and aggregation, decreases coronary blood flow. Plaques with thinner fibrous caps are more “vulnerable” to rupture.
Myocardial ischemia also may be silent, with electrocardiographic, echocardiographic, or radionuclide evidence of ischemia appearing in the absence of symptoms. While some patients have only silent ischemia, most patients who have silent ischemia have symptomatic episodes as well. The precipitants of silent ischemia appear to be the same as those of symptomatic ischemia. We now know that the ischemic burden, i.e., the total time a patient is ischemic each day, is greater in many patients than was recognized previously. In most trials, the agents that are efficacious in conventional angina are also efficacious in reducing silent ischemia. b Adrenergic receptor antagonists appear to be more effective than the Ca2+ channel blockers in the prevention of episodes.
Therapy directed at abolishing all silent ischemia has not been shown to be of additional benefit over conventional therapy.
The major drugs are nitro vasodilators, b adrenergic receptor antagonists, Ca2+ channel antagonists, and in stable and unstable angina, antiplatelet agents as well as statins (HMG CoA-reductase inhibitors), which may have a role in stabilizing the vulnerable plaque. All approved antianginal agents improve the balance of myocardial oxygen supply and demand, increasing supply by dilating the coronary vasculature or decreasing demand by reducing cardiac work. Increasing the cardiac extraction of oxygen from the blood is not a practical therapeutic goal.
Drugs used in typical angina function principally by reducing myocardial oxygen demand by decreasing heart rate, myocardial contractility, and/or ventricular wall stress. Patients with mild or moderate stable angina, who do not have left ventricular dysfunction, may be managed effectively with sublingual glyceryl trinitrate and regular administration of a beta-blocker. If necessary a long-acting dihydropyridine calcium-channel blocker and then a long-acting nitrate may be added. For those without left ventricular dysfunction and in whom beta-blockers are inappropriate, diltiazem or verapamil may be given and a long-acting nitrate may be added if symptom control is not adequate. For those intolerant of standard treatment, or where standard treatment has failed, nicorandil may be tried.
For angina in patients with left ventricular dysfunction a long-acting nitrate or a long-acting dihydropyridine calcium-channel blocker, such as amlodipine or felodipine should be used alone, or in combination, to prevent clinical deterioration; nicorandil can also be considered as an alternative treatment. Increasingly, a beta-blocker is also used in clinically stable patients; treatment should be started at a very low dose and titrated very slowly over a period of weeks or months.
By contrast, the principal therapeutic goal in unstable angina is to increase myocardial blood flow; strategies include the use of antiplatelet agents and heparin to reduce intracoronary thrombosis and coronary stents or coronary bypass surgery to restore flow by mechanical means. The therapeutic aim in variant or Prinzmetal angina is to prevent coronary vasoplasm.
Antianginal agents may provide prophylactic or symptomatic treatment, but b adrenergic receptor antagonists also reduce mortality apparently by decreasing the incidence of sudden cardiac death associated with myocardial ischemia and infarction. The treatment of cardiac risk factors can reduce the progression or even lead to the regression of atherosclerosis. Aspirin is used routinely in patients with myocardial ischemia, and daily aspirin use reduces the incidence of clinical events. Other antiplatelet agents such as oral clopidogrel and intravenous anti-integrin drugs such as abciximab, tirofiban, and eptifibatide have been shown to reduce morbidity in patients with angina who undergo coronary artery stenting.
Lipid-lowering drugs such as the statins reduce mortality in patients with hypercholesterolemia with or without known coronary artery disease. Angiotensin-converting enzyme (ACE) inhibitors also reduce mortality in patients with coronary disease. Coronary artery bypass surgery and percutaneous coronary interventions such as angioplasty and coronary artery stent deployment can complement pharmacological treatment. In some subsets of patients, percutaneous or surgical revascularization may have a survival advantage over medical treatment alone. Intracoronary drug delivery using drug-eluting coronary stents represents an intersection of mechanical and pharmacological approaches in the treatment of coronary artery disease. Novel therapies that modify the expression of vascular or myocardial cell genes eventually may become an important part of the therapy of ischemic heart disease.
By: Ammarah Khan



